A throbbing tooth that won’t let up can change the whole day. Eating hurts, sleep gets interrupted, and a small spot in the mouth starts to feel like a much bigger problem. Many people searching for an emergency dentist near me in Amanda, OH, Lancaster, OH, Circleville, OH, or Carroll, OH are in exactly that position. They’re trying to decide whether the pain can wait or whether it signals something more serious.
When the cause is a dental abscess, the answer is simple. It shouldn’t be ignored. An abscessed tooth is an infection, not just irritation, and complications from abscessed tooth problems can move from pain and swelling to wider health concerns if treatment is delayed. The good news is that this is a serious but manageable condition. Prompt dental care can relieve pressure, stop the spread of infection, and protect both short-term comfort and long-term health.
Table of Contents
- Your Trusted Emergency Dentist for Amanda and Lancaster OH
- Understanding a Dental Abscess Beyond a Simple Toothache
- Local Complications When an Abscess Spreads Nearby
- Systemic Dangers Serious Complications from an Abscessed Tooth
- Emergency Warning Signs That Require Immediate Dental Care
- How Amanda Family Dental Treats an Abscessed Tooth
- Schedule Your Appointment and Prevent Future Emergencies
Your Trusted Emergency Dentist for Amanda and Lancaster OH
A common pattern starts the same way. A tooth feels sensitive for a few days, then the pain becomes sharp or throbbing. By the time swelling shows up in the gums or cheek, many people have already tried rinses, pain relievers, or waiting it out, hoping the problem settles down on its own.
That’s where an abscess often misleads people. The pain may briefly ease if pressure shifts or drainage occurs, but the infection itself usually hasn’t gone away. It remains active, and that’s why the right next step is an urgent dental evaluation rather than another day of hoping.
For families in Amanda, Lancaster, Circleville, and Carroll, this matters because dental infections rarely improve through guesswork. A serious toothache can affect work, school, sleep, and meals within a day or two. It can also create anxiety fast, especially when facial swelling starts or chewing becomes difficult.
Practical rule: A toothache that is worsening, throbbing, or paired with swelling should be treated like an infection until a dentist proves otherwise.
An emergency dentist’s role isn’t just to reduce pain. Their primary responsibility involves finding the source, checking whether the infection is contained or spreading, and choosing the treatment that effectively solves the problem. That may mean draining an abscess, prescribing antibiotics when they’re indicated, performing a root canal, or removing a tooth that can’t be predictably saved.
What urgent care should accomplish
| Immediate problem | What effective dental care does |
|---|---|
| Pressure and throbbing | Relieves the trapped infection and pressure |
| Uncertain cause | Uses an exam and dental X-rays to locate the source |
| Swelling | Assesses whether the infection is staying local or spreading |
| Fear of losing the tooth | Compares root canal treatment with tooth extraction |
| Risk of recurrence | Plans follow-up restoration and prevention |
A calm, timely visit changes the trajectory. Instead of allowing the infection to keep building, treatment moves the situation back into control and protects the rest of the mouth and body.
Understanding a Dental Abscess Beyond a Simple Toothache
A dental abscess is a pocket of infection. It's similar to an infected splinter that the body has tried to wall off. The problem is that the source remains trapped in a place that won’t heal cleanly without professional treatment.
Pain happens because pressure builds inside the tooth or the surrounding tissues. Nerves become irritated, the area gets inflamed, and biting down can feel surprisingly intense. Some patients notice a foul taste, gum swelling, or sensitivity to hot and cold. Others mainly notice that one tooth suddenly feels “high” or sore when they close their mouth.
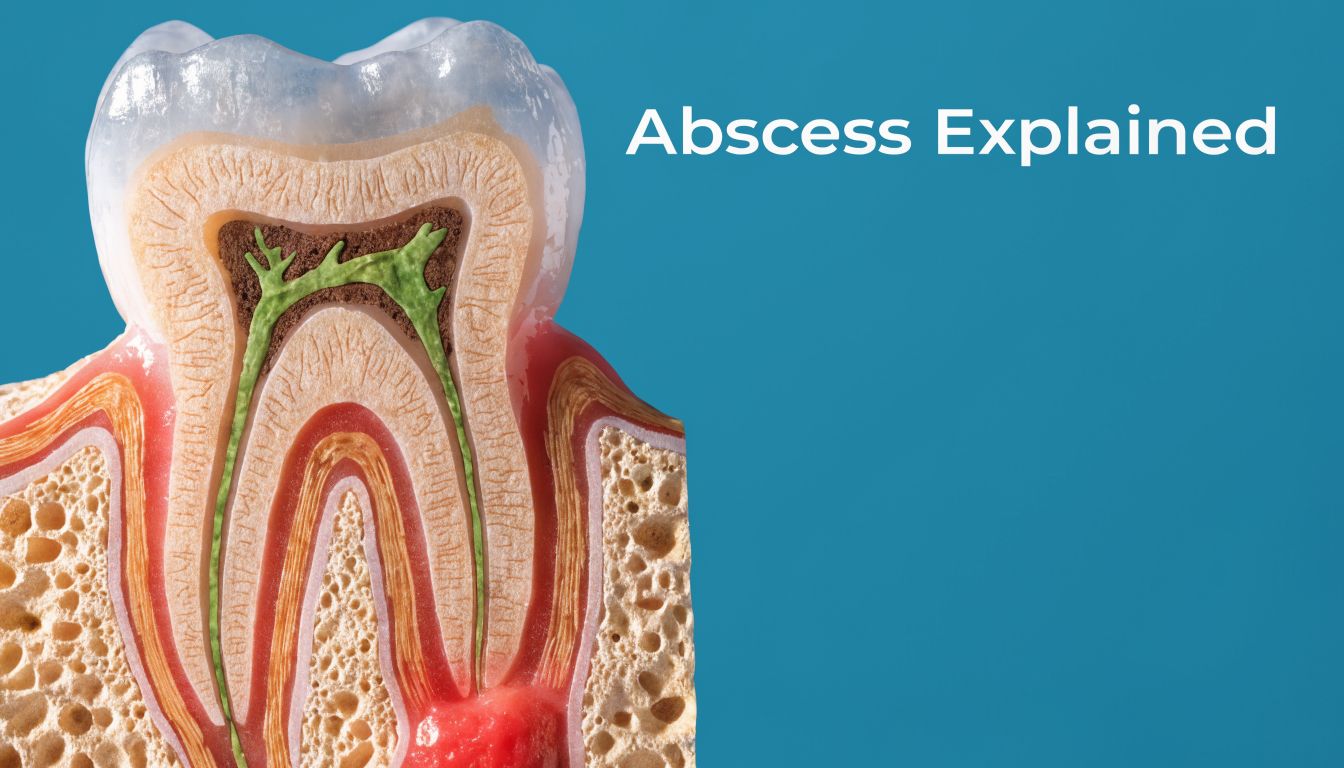
What an abscess actually is
An abscess usually forms when bacteria enter an area they shouldn’t be able to reach. That can happen after untreated decay, a crack, trauma, or advanced gum problems. Once bacteria reach deeper tissues, the body responds with inflammation and infection.
This is why home remedies have limits. Warm saltwater rinses may soothe irritated tissue. Cold compresses may reduce discomfort. Over-the-counter pain relievers may help someone get through the night. None of those removes infected pulp, drains a deep pocket, or seals the route that let bacteria in.
An abscess can quiet down temporarily without actually resolving. That’s one reason people are often surprised when the pain returns stronger.
Two common types patients hear about
A periapical abscess forms near the tip of the tooth root. This type often starts inside the tooth, where decay or damage reaches the pulp. Patients often describe deep, pounding pain and tenderness when biting.
A periodontal abscess forms in the gums around a tooth. This type is often linked to gum infection or a trapped area where bacteria collect beside the root. Patients may notice a swollen gum bump, tenderness in one spot, or drainage with a bad taste.
A simple comparison helps:
- Periapical abscess usually starts inside the tooth
- Periodontal abscess usually starts in the supporting gum tissues
- Both types involve active infection and need treatment
- Neither type should be expected to heal fully without dental care
For anyone searching for a dentist in Amanda, OH or an emergency dentist near Lancaster, OH, the main takeaway is straightforward. If there’s an abscess, the primary concern isn’t just pain. It’s an infection that needs to be evaluated, contained, and definitively treated.
Local Complications When an Abscess Spreads Nearby
The first complications from abscessed tooth infections usually stay close to where the problem started. That doesn’t make them minor. Local spread can damage the tissues that support the tooth and make treatment more involved if it’s delayed.
When bacteria move beyond the original tooth, they can irritate the gums, surrounding bone, and nearby soft tissues. The spread of bacteria from dental abscesses can form dental cysts at the base of the gums and accelerate gum disease, which complicates eating and overall health, as noted in this discussion of abscess-related spread. That’s one reason early intervention matters.
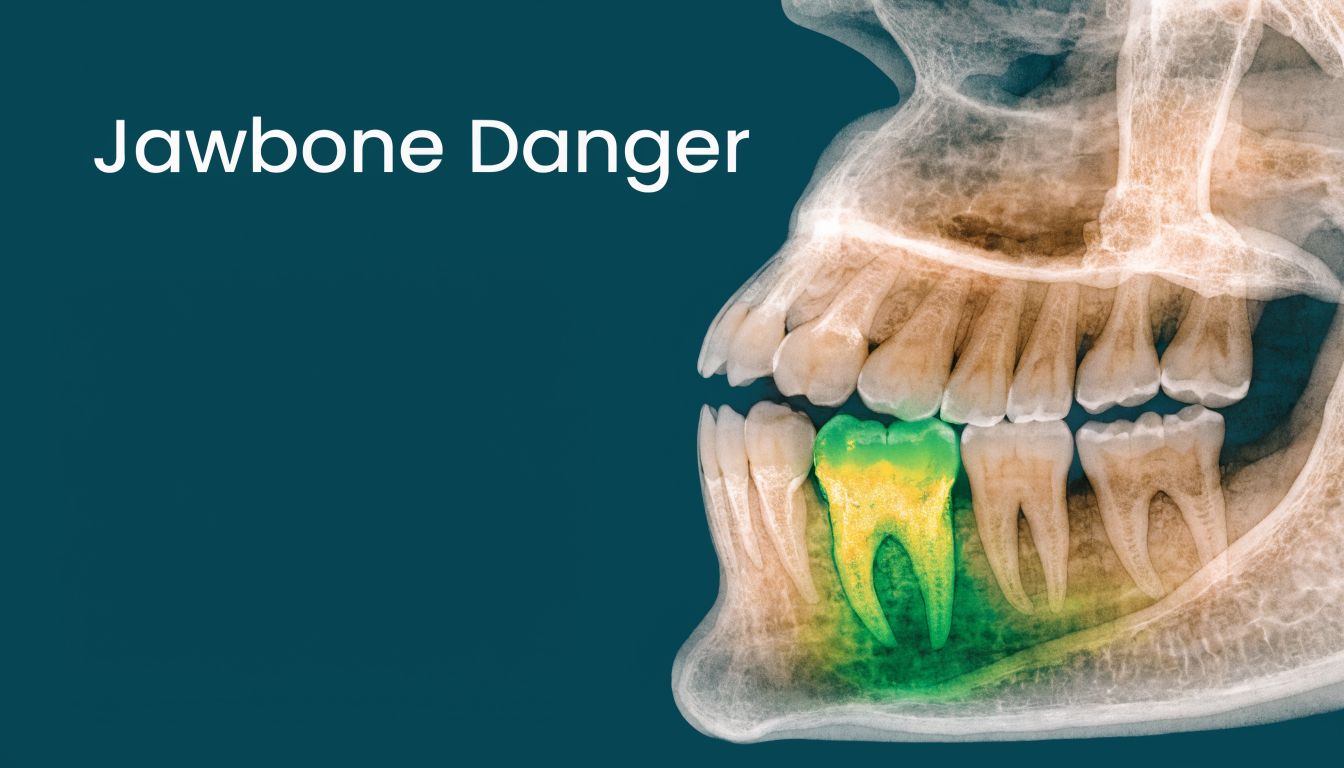
What happens in the gums and jaw
Bone loss is one of the most important local concerns. Chronic infection can weaken the bone around a tooth, making that tooth less stable and reducing future treatment options. In practical terms, the longer the infection remains active, the harder it can become to save the tooth or restore the area.
Nearby tissues can also become swollen and tender. Some patients develop facial cellulitis, where skin and deeper soft tissues of the face or jaw become red, warm, and painful. Others notice the swelling shifting toward the cheek, the floor of the mouth, or under the jawline.
A short pattern list helps patients identify what’s changing:
- Jaw soreness that spreads beyond one tooth
- Visible gum swelling or a pimple-like bump near the tooth
- Pain with chewing because pressure inflames the area
- Facial fullness on one side
- Worsening tenderness despite self-care
When pain starts affecting the face and daily life
Upper tooth infections can also irritate nearby sinus spaces. Patients sometimes think they have a sinus problem first because they feel pressure in the cheek, tenderness around the upper back teeth, or discomfort that worsens when bending forward.
Managing discomfort at home can help someone get to an appointment more comfortably, but it doesn’t replace care. For people trying to distinguish tooth-related soreness from other facial or jaw discomfort, this guide to medication options for muscle discomfort can be useful background. If the source is an abscess, though, pain relief alone won’t fix it.
For patients who also notice head pressure with a painful tooth, abscessed tooth headache symptoms and causes can help connect the dots. A headache, cheek pressure, or jaw pain may all be coming from the same infected tooth.
Systemic Dangers Serious Complications from an Abscessed Tooth
An abscessed tooth can start with pain in one spot and end up affecting systems far beyond the mouth. Once bacteria break past the tooth and surrounding tissues, the problem can involve the airway, the bloodstream, and organs that seem unrelated to dental health.
For families in Amanda, this matters for more than the current emergency. Ongoing oral infection adds inflammatory stress to the body. In patients already managing diabetes, heart disease, or a weakened immune system, that extra burden can make recovery harder and daily health less stable. The American Heart Association has also noted important links between oral health and cardiovascular health in its overview of how oral health and heart health connect.
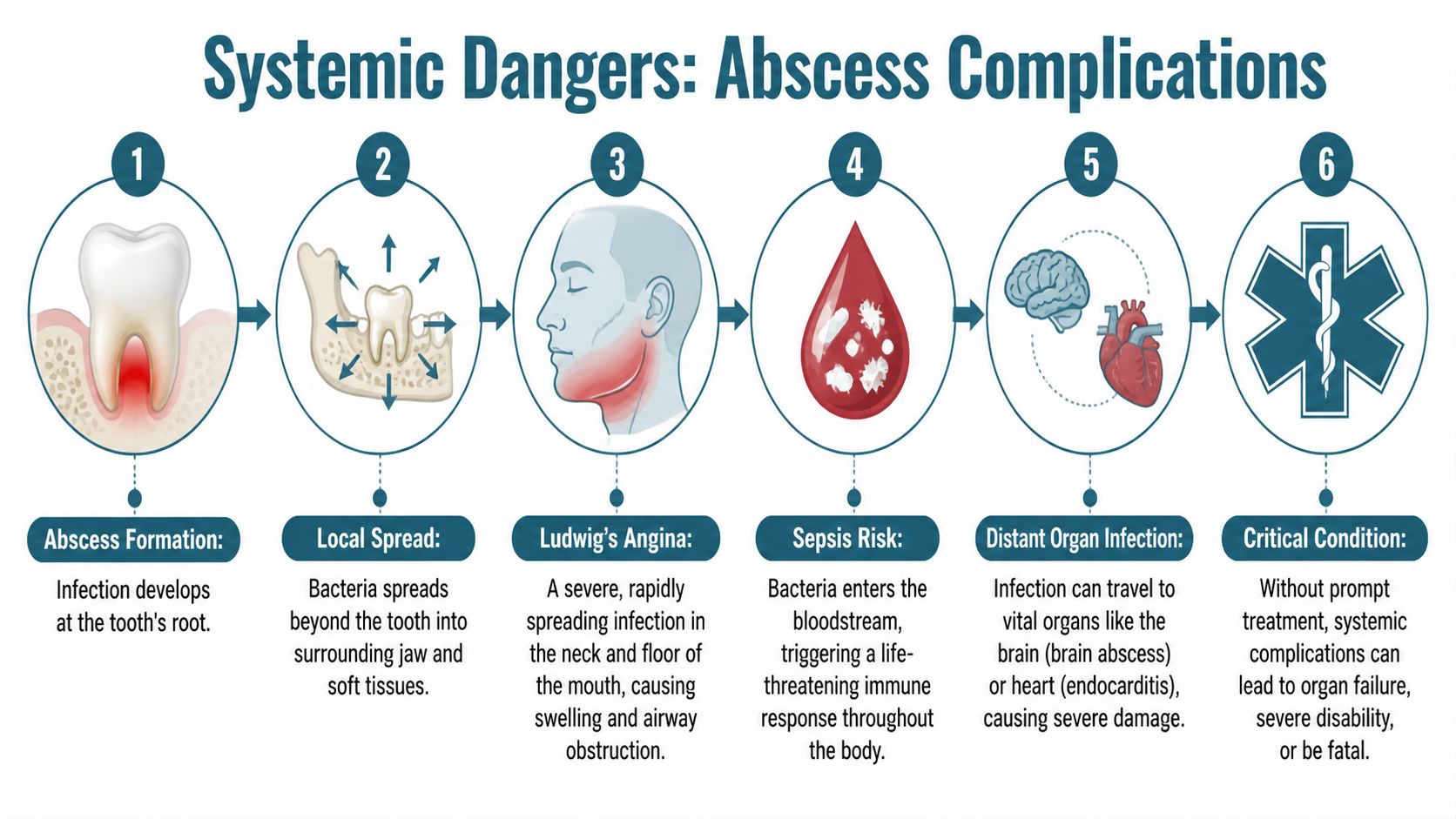
How a dental infection spreads beyond the mouth
One serious complication is Ludwig’s angina, an infection that involves the floor of the mouth and tissues under the jaw. The danger is mechanical as much as infectious. Swelling in that area can raise the tongue and reduce the airway space, which is why these cases sometimes need hospital care and airway support, as described in the MSD Manual overview of dental emergencies.
Sepsis is another concern. If bacteria enter the bloodstream, the body can respond with widespread inflammation, low blood pressure, and organ stress. Patients often ask whether a tooth infection can really do that. It can. If you want a clearer explanation of how an oral infection can spread through the body, our page on blood infection from a tooth abscess explains what to watch for and why timing matters.
Some infections also travel into deep spaces of the head, neck, or chest. MedlinePlus warns that an untreated tooth abscess can lead to spread into surrounding tissues and other parts of the body, which is why delay is risky even when pain briefly improves, according to its patient resource on tooth abscess complications and treatment.
Why this section matters for long-term family health
In practice, the immediate goal is to stop the infection and relieve pressure. The longer-term goal is to protect overall health and prevent the same cycle from affecting other family members. A parent who delays care because the pain comes and goes may end up needing more invasive treatment later. A grandparent with heart or immune problems faces a different set of risks than a healthy teenager. The treatment plan should account for those trade-offs.
That is why prompt dental care protects more than one tooth. It helps reduce the chance of repeat infections, limits inflammation, and keeps a localized problem from turning into a broader health issue that disrupts work, school, sleep, and medical conditions already being managed.
If you are unsure whether symptoms belong in a dental office, an ER, or another setting, this urgent care decision guide can help with general triage. For a suspected abscess, the source still needs dental treatment. At Amanda Family Dental, we focus on removing the infection, preserving teeth when possible, and restoring a healthier baseline for patients and families across Amanda and Lancaster.
Emergency Warning Signs That Require Immediate Dental Care
A parent wakes up with a swollen jaw, plans to get through work first, and by lunchtime swallowing feels tight. That is the point where a dental problem may be turning into a medical emergency. With an abscess, the pattern matters as much as the pain.

Red flags that should not wait
Call for immediate dental or hospital care if you notice any of the following:
- Swelling that is spreading into the cheek, jaw, eye area, or neck
- Trouble swallowing or pressure in the throat
- Breathing difficulty or swelling under the tongue or floor of the mouth
- Fever with dental pain, especially with facial swelling
- Vision changes or swelling around the eye
- Confusion, unusual drowsiness, or feeling faint
- Severe, constant pain that keeps worsening
These signs suggest the infection may be moving beyond the tooth and gum. At that stage, the goal is no longer just pain relief. The priority is protecting the airway, limiting deeper spread, and getting the right level of care quickly.
Urgency check: If swelling affects breathing, swallowing, eye symptoms, or mental status, get emergency medical evaluation right away.
When to call a dentist and when to go to the hospital
If the problem is intense tooth pain, gum swelling, bad taste or drainage, or pain with chewing, an emergency dental visit is often the right first step. Our office can examine the area, take X-rays, relieve pressure, and decide whether the tooth can be saved. If treatment may involve endodontic care, patients often feel more prepared after reading about how to prepare for a root canal.
Hospital care is the safer choice when swelling is spreading into the face or neck, fever is rising, the person feels weak or ill overall, or there is any concern about breathing or swallowing. Patients with diabetes, heart conditions, cancer treatment, or immune suppression should be especially cautious. In those families, an abscess can affect more than one difficult day. It can interfere with medical stability, delay recovery, and add inflammatory stress to conditions already being managed.
For patients deciding between office care and medical urgent care, this urgent care decision guide offers a helpful general framework. In Amanda and Lancaster, we want families to know they do not need to guess alone. Prompt evaluation protects the tooth when possible, and it also helps protect long-term oral and overall health for every generation in the household.
A brief explainer can also help clarify what worsening infection can look like:
How Amanda Family Dental Treats an Abscessed Tooth
An abscessed tooth needs more than pain relief. The infection has to be brought under control, the pressure has to be reduced, and the source has to be treated in a way that protects your health long term.
At our Amanda practice, we start by finding out exactly what is happening. A clinical exam and digital X-rays show whether the infection is centered inside the tooth, around the root, or affecting the surrounding bone and gum tissue. That matters because the right treatment for a restorable tooth is different from the right treatment for a tooth that is too damaged to keep.
The first step is often to relieve pressure and reduce the bacterial burden. If pus has collected, drainage may be needed to ease pain and help the area calm down. Antibiotics may also be prescribed when swelling is spreading, nearby tissues are involved, or a patient has medical risk factors that make infection harder to contain. Antibiotics help in the right cases, but they do not remove dead tissue from inside a tooth or repair a badly broken tooth. Without definitive treatment, the infection often returns.
From there, treatment usually falls into two paths:
- Root canal treatment if the tooth can be saved and restored predictably
- Extraction if the tooth is too broken down, too loose, or unlikely to do well even after treatment
A root canal removes infected tissue from inside the tooth, cleans the canal space, and seals it to reduce the chance of reinfection. For many patients, this is the best balance of infection control, comfort, and long-term function because it preserves the natural tooth and helps maintain normal chewing. Patients who want a clearer sense of what that visit involves can review what to expect and how to prepare for a root canal.
Extraction is sometimes the safer choice. If a tooth cannot be restored well, keeping it can lead to repeated infections, more bone loss, and more costly treatment later. Removing the source of infection allows healing to begin. After that, we can talk through practical replacement options such as a bridge, denture, or implant, based on age, bone support, budget, and the needs of the rest of the bite.
That decision is not just about one painful tooth. For parents, grandparents, and adults managing conditions such as diabetes or heart concerns, controlling oral infection can reduce one more source of ongoing inflammatory stress. Good treatment now also helps protect nearby teeth, preserve bone, and keep future care simpler for the whole family.
My advice is straightforward. Treat the abscess early, choose the option that gives the most predictable result, and finish the recommended follow-up care. Prompt treatment usually turns a serious problem into a manageable one.
Schedule Your Appointment and Prevent Future Emergencies
A tooth abscess is painful in the moment, but the longer-term picture matters too. Untreated abscesses can lead to chronic issues like gum disease and bone loss, which can weaken the jaw and complicate future restorative options like dental implants or dentures, as discussed in this overview of serious abscess complications and prevention. That’s one reason early care protects more than a single tooth.
For families, prevention becomes practical. Regular cleanings and exams help catch decay, cracks, gum problems, and failing dental work before they turn into infection. Children benefit because small problems can be treated early. Adults benefit because preserving bone, gum support, and healthy bite function makes future restorative care much simpler.
Why prevention matters for the whole family
A prevention-focused approach supports more than comfort:
- Protects chewing function so meals stay comfortable and balanced
- Reduces long-term damage to gums, bone, and nearby teeth
- Supports restorative choices if a crown, root canal, implant, or denture is ever needed
- Helps the whole household stay ahead of emergencies through routine visits
The smartest time to deal with an abscess risk is before it becomes an emergency. That means addressing tooth pain early, keeping up with dental X-rays and exams, and treating infection before it affects the rest of the mouth or body.
For patients in Amanda, OH, Lancaster, OH, Circleville, OH, and Carroll, OH, fast treatment and steady preventive care work together. One stops today’s pain. The other helps keep the same problem from returning.
If dental pain, swelling, or pressure is starting to feel like more than a routine toothache, schedule an appointment with Amanda Family Dental. The practice provides family dentistry, emergency dental services, root canals, tooth extraction, restorative care, and preventive exams for patients in Amanda, Lancaster, Circleville, and Carroll, Ohio.
