A person in Amanda, Lancaster, Circleville, or Carroll, Ohio often starts in the same place. A tooth hurts, then the pain lingers into the night, the gum looks puffy, and the question changes from “Can this wait?” to “Could this be serious?”
That concern is reasonable. A blood infection from tooth abscess sounds extreme, but the basic idea is simple. An infection that begins inside a tooth can sometimes move beyond the tooth and affect the rest of the body. That doesn't happen in every case, and modern treatment is very effective, but it does mean a severe tooth infection shouldn't be brushed off as “just dental pain.”
This is where many people get stuck. They aren't sure whether they need an emergency dentist, a next-day dental visit, or the emergency room. They also may not know which warning signs point to a local problem and which signs suggest the infection may be spreading.
Table of Contents
- That Worsening Toothache Could Be a Serious Warning
- How a Tooth Infection Spreads to Your Blood
- Emergency Symptoms of a Spreading Tooth Infection
- Your Treatment Path Dentist vs Emergency Room
- Definitive Dental Solutions at Amanda Family Dental
- Are You at Higher Risk? Prevention and Personalized Care
- Frequently Asked Questions About Tooth Abscesses
That Worsening Toothache Could Be a Serious Warning
A common pattern starts small. A person notices a dull ache while chewing on one side. By evening, the tooth throbs. The next morning, cold water stings, the gum feels tender, and there may be a bad taste in the mouth. At that point, many people still hope it will settle down on its own.
Sometimes it doesn't. The pain gets sharper, sleep gets harder, and swelling starts to show. What felt like a routine cavity begins to feel different. That change matters.
When tooth pain stops being routine
A severe toothache can mean the inside of the tooth is infected. If pus collects, that infection becomes an abscess. Left alone, it can move into nearby tissues and create a larger problem than pain alone.
Dental infections send enough people to the hospital that they occur at a rate of about 1 per 2,600 people in the United States, according to a source cited in this review of sepsis from tooth infection. That doesn't mean every toothache turns dangerous. It does mean worsening symptoms deserve prompt attention.
Practical rule: Pain that is intensifying, waking someone from sleep, or coming with swelling is not a “watch and wait” situation.
People also get confused when the painful tooth already had treatment before. A prior filling or root canal can make the situation feel less obvious. For readers trying to make sense of lingering or renewed symptoms after earlier dental work, this guide on understanding post-root canal complications can help clarify why a tooth may still need evaluation.
Clues the infection may be building
Some signs point toward an abscess rather than ordinary sensitivity:
- Throbbing pain: The ache tends to pulse and may spread into the jaw, ear, or temple.
- Swollen gum: A bump on the gum or fullness near one tooth can signal trapped infection.
- Bad taste or drainage: Pus may drain into the mouth and create a foul taste.
- Pain with pressure: Biting down can feel sharply worse.
Head pain can add another layer of confusion. A dental abscess can refer pain upward and feel like a sinus issue or headache. This explanation of how an abscessed tooth can trigger headache symptoms helps connect those dots.
The key point is reassuring and direct at the same time. Most tooth infections can be treated successfully when care happens early. Trouble starts when a person delays treatment long enough for the infection to move beyond the tooth.
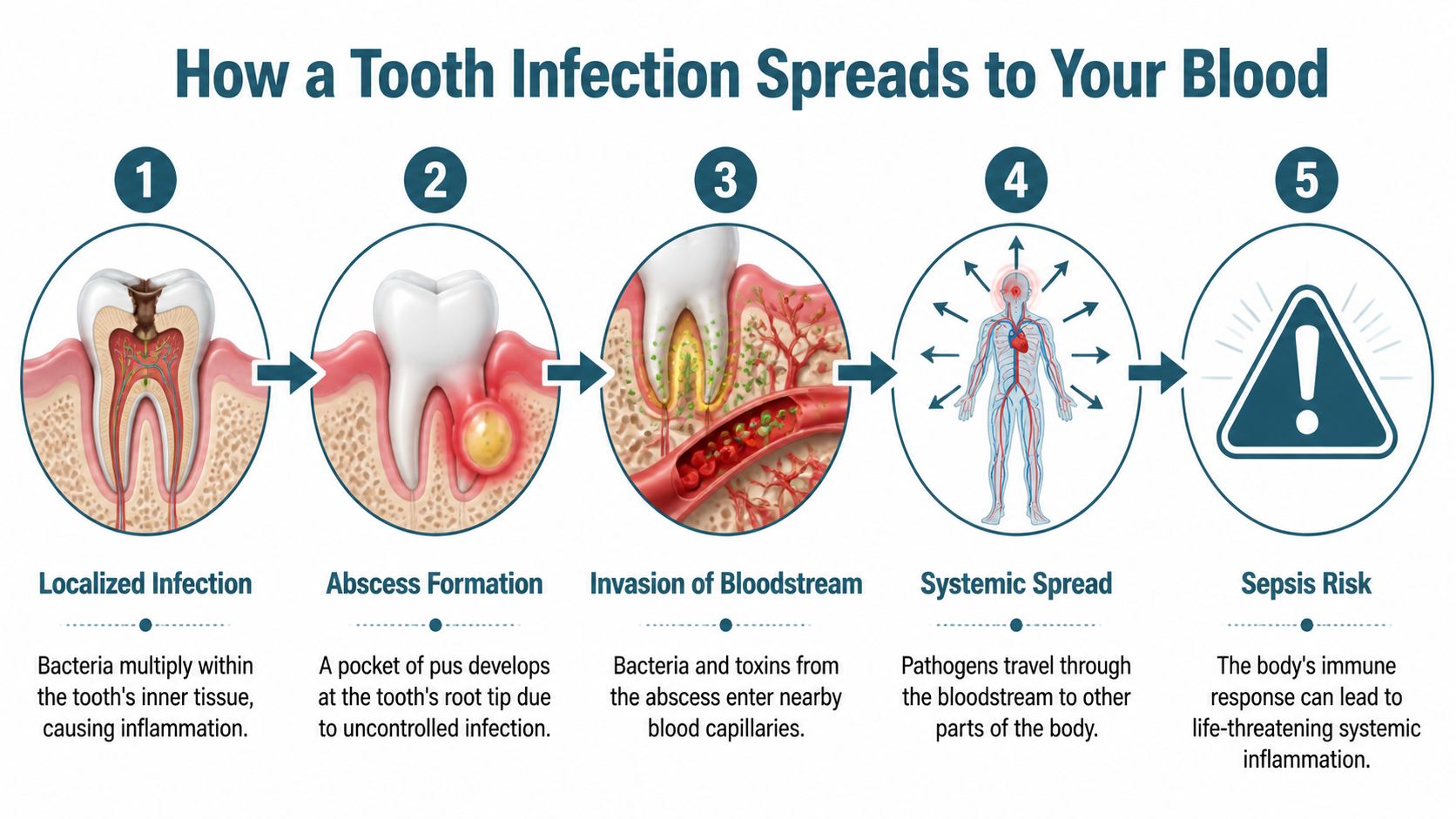
How a Tooth Infection Spreads to Your Blood
A tooth doesn't look connected to the rest of the body in an obvious way, which is why this topic feels strange to many patients. But each tooth contains living tissue, and that tissue sits next to blood vessels, bone, and soft tissue. Once infection breaks out of the tooth, it has a path to travel.
What an abscess actually is
A tooth abscess is a pocket of infection, usually caused by bacteria that entered the pulp through decay, trauma, or other damage. These infections are often polymicrobial, which means more than one type of bacteria is involved. A microbiology review notes that dental abscesses often include anaerobic bacteria such as Prevotella and Fusobacterium, and that these organisms can breach the tooth's anatomy and enter the bloodstream, potentially leading to sepsis, as described in this NCBI article on odontogenic infections.
That sounds technical, but the plain-language version is straightforward. Bacteria get into the center of the tooth. The body reacts. Pressure builds. Pus forms. If the infection isn't drained or treated, it looks for somewhere else to go.
How bacteria move beyond the tooth
A helpful way to picture it is a leak behind a wall. At first, the problem is hidden and local. Then the pressure rises, the material spreads into nearby spaces, and damage reaches places that weren't part of the original problem.
The spread often follows this pattern:
- The pulp becomes infected. This is the soft inner area with nerves and blood supply.
- An abscess forms. Pus collects near the root tip or gum.
- Nearby tissue gets involved. Swelling can move into the face or jaw.
- Bacteria reach the bloodstream. This is called bacteremia, meaning bacteria are present in the blood.
- The body overreacts. That severe body-wide response is sepsis.
Bacteremia means bacteria have entered the blood. Sepsis means the body's response to infection is harming the body itself.
People often confuse these terms. Not every bloodstream exposure becomes sepsis. But once there are body-wide symptoms such as fever, confusion, or low blood pressure, the situation has moved well beyond a routine dental issue.
A blood infection from tooth abscess is serious because the mouth sits close to deep tissues of the face, jaw, and neck. That closeness is one reason dentists take swelling so seriously, especially when it begins to spread or affects swallowing, speech, or breathing.
Emergency Symptoms of a Spreading Tooth Infection
Knowing the mechanism helps, but symptoms are what drive real-life decisions. A person doesn't need to identify bacteria or understand anatomy in the moment. That person needs to know which signs mean “call a dentist now” and which signs mean “go to the ER now.”

Red flags that change this into a medical emergency
According to Sepsis Alliance guidance on dental health and sepsis, sepsis from a dental source is a medical emergency. Warning signs that need immediate ER evaluation include a high fever over 101°F, heart rate over 100 beats per minute, confusion, and severe facial or neck swelling.
Those aren't routine tooth infection symptoms. They suggest the problem may be affecting the body as a whole.
A practical checklist looks like this:
- High fever: Not just feeling warm, but a true fever over 101°F.
- Fast heart rate: A pounding or racing pulse over 100 beats per minute.
- Confusion or unusual sleepiness: Trouble thinking clearly is never a dental-office waiting symptom.
- Severe facial or neck swelling: Especially if swelling is spreading, tightening, or affecting swallowing.
- Breathing trouble: This needs emergency care immediately.
Symptoms people sometimes dismiss by mistake
Some people delay care because the symptom doesn't “feel dental.” They may focus on chills, weakness, dizziness, or a sick-all-over feeling and miss the connection to the infected tooth.
That can happen with dizziness as well. This overview of whether an abscessed tooth can cause dizziness helps explain why a dental infection can create symptoms that seem unrelated at first.
A blood test may also show the body is fighting infection. For readers curious about that lab result, this explanation of what high white blood cells mean gives useful background on why the count can rise during infection.
This short video also gives a helpful overview of warning signs and urgency:
If a tooth hurts and the person also has fever, confusion, or rapidly spreading swelling, the safest assumption is that this is no longer just a tooth problem.
A simple toothache can wait for a scheduled visit in some cases. Systemic symptoms should not.
Your Treatment Path Dentist vs Emergency Room
Many families lose time at this stage. They know something is wrong, but they aren't sure where to go first. The right answer depends on whether the infection still appears localized or whether it has become systemic.

A useful source on this distinction explains that localized swelling and pain warrant an urgent dental visit for source control, while systemic signs like fever and confusion demand immediate ER care, and that many patients are left unsure of that first step. That guidance appears in this article on signs of tooth infection spread to blood.
When a dentist is the right first call
If the symptoms are concentrated around the tooth, the dentist is usually the right starting point. This includes problems such as visible gum swelling near one tooth, pain when biting, bad taste from drainage, or a clear abscess with no body-wide illness.
A dentist treats the source. That matters because antibiotics alone often don't solve the entire problem if infected tissue or trapped pus remains.
| Situation | Best first step | Why |
|---|---|---|
| Throbbing tooth pain with localized gum swelling | Urgent dental visit | The tooth likely needs drainage, root canal treatment, extraction, or other direct treatment |
| Bad taste or pus near one tooth | Urgent dental visit | The infection source is in the mouth and needs dental treatment |
| Painful biting pressure without fever or confusion | Urgent dental visit | The issue may still be localized |
When the emergency room is the right first stop
The ER becomes the right choice when the body is showing signs it may be under broader stress from infection. The hospital can evaluate airway risk, give IV fluids, provide urgent medical support, and manage severe infection.
These situations call for the ER first:
- Fever with tooth infection: Especially when paired with swelling or weakness.
- Confusion or faintness: Mental changes aren't routine dental symptoms.
- Swelling into the face or neck: This raises concern about deeper tissue spread.
- Trouble breathing or swallowing: This is urgent immediately.
- A racing heartbeat with feeling very ill: That combination should not wait.
A dentist removes the dental source. An emergency room manages body-wide danger. Some patients need both, in that order.
For people trying to secure urgent dental help quickly after the emergency issue is stabilized, this guide on find same day emergency dentists may be useful.
The most important thing is speed, not perfection. If symptoms are clearly systemic, the ER is the safer choice. If the problem is still local, fast dental care is the move that can stop it from getting worse.
Definitive Dental Solutions at Amanda Family Dental
Once the immediate danger is sorted out, the infected tooth still needs treatment. That part matters just as much. If the source remains in place, the pain can return and the infection can flare again.
Why the source of the infection must be treated
Before antibiotics were widely available, the fatality rate from a spreading tooth infection could be as high as 40%, according to this review of whether a tooth infection can spread to the blood. Today, modern dental care has changed that picture dramatically. Root canals, extractions, drainage, and antibiotics are highly effective at stopping the infection where it starts.
That is why “just take antibiotics” isn't the full answer in many cases. Medication can help reduce bacterial spread, but a dentist often still needs to remove infected pulp, drain the abscess, or remove a tooth that can't be saved.
Common treatments that stop the problem
The right treatment depends on the tooth and how far the infection has progressed. Common solutions include:
- Abscess drainage: Releasing trapped pus lowers pressure and reduces pain.
- Root canal treatment: The infected tissue inside the tooth is removed, the canals are cleaned, and the tooth is sealed.
- Tooth extraction: If the tooth can't be predictably saved, removing it can be the safest way to eliminate the source.
- Antibiotics as support: These may be used along with dental treatment, especially when swelling or spread is a concern.
For patients considering whether a painful infected tooth may be saved rather than removed, this page on root canal treatment options offers a useful overview.
A lot of fear comes from the word “procedure.” In reality, the procedure is often the part that starts the relief. Once pressure is reduced and the infection source is addressed, many patients feel a major shift in comfort.
Are You at Higher Risk? Prevention and Personalized Care
Not every person faces the same level of risk from the same infection. That matters because it changes how quickly someone should act on swelling, pain, or drainage.
Who needs faster action
People with diabetes, HIV, heart disease, or other immunocompromising conditions are at a significantly higher risk for a dental abscess to progress to a severe systemic infection, according to this discussion of early sepsis signs from a tooth infection.
That doesn't mean every infected tooth in a higher-risk patient becomes dangerous. It means the margin for delay is smaller.
A few examples help make that clearer:
- A healthy adult with localized tooth pain still needs prompt care, but may not have the same risk profile as someone medically fragile.
- A person with diabetes and facial swelling should move faster because healing and infection control may be harder.
- An older adult with heart disease and fever shouldn't treat the problem like an ordinary toothache.
Higher-risk patients shouldn't wait for symptoms to become dramatic before seeking help.
How prevention lowers risk
Prevention is less about “perfect teeth” and more about stopping small problems before bacteria reach the pulp. Regular exams, dental X-rays when needed, early treatment of decay, and fast attention to cracked teeth all reduce the chance that an abscess will form.
The same is true after dental work. If pain returns, swelling appears, or a tooth feels wrong after treatment, follow-up matters. The safest pattern is simple. Catch problems early, treat the cause directly, and act faster when medical risk factors are present.
Frequently Asked Questions About Tooth Abscesses
Can a tooth infection go away on its own
It may seem to calm down for a short time, especially if pressure changes or drainage starts, but the infection itself usually doesn't resolve without treatment. A quiet phase can be misleading.
If someone is taking antibiotics, is that enough
Often, no. Antibiotics may help control the infection, but a dentist may still need to drain the abscess, perform a root canal, or remove the tooth. The source has to be addressed.
How quickly can a blood infection from tooth abscess happen
There isn't one fixed timeline. Some infections stay local for a while. Others worsen more quickly, especially in people with higher medical risk or when swelling is spreading.
What if the face looks swollen but there is no fever
That still needs urgent dental attention. Facial swelling means the infection is moving beyond the tooth. If the swelling increases, reaches the neck, or comes with fever, confusion, or trouble swallowing, emergency care is the safer move.
Is a root canal better than an extraction
When a tooth can be predictably saved, a root canal is often a good option because it removes infection while keeping the natural tooth. If the tooth is too damaged, extraction may be the better solution.
When should a family stop reading and call for help
If there is severe pain with swelling, call a dentist promptly. If there is fever, confusion, severe swelling of the face or neck, or trouble breathing or swallowing, go to the ER.
Families dealing with tooth pain, swelling, or a possible dental abscess in Amanda, OH, Lancaster, OH, Circleville, OH, or Carroll, OH don't have to guess their way through it. Amanda Family Dental provides patient-focused dental care, including exams, digital X-rays, emergency dental services, tooth extraction, restorative treatment, and root canal care. For anyone searching for a dentist near me, an emergency dentist, or a dentist in Amanda, OH, reaching out promptly is the best next step.