Yes, an abscessed tooth can cause dizziness, and research indicates that people with untreated dental infections have a 30% higher risk of experiencing dizziness than those without infection. It’s a real medical connection, not an unusual coincidence, and it usually comes down to inflammation, sinus pressure, nearby balance structures, and the strain that pain and infection put on the body.
That can feel alarming when someone is already dealing with a throbbing tooth, a bad taste in the mouth, or pressure in the face and then suddenly starts feeling lightheaded or off balance. Many people in Amanda, Lancaster, Circleville, and Carroll, Ohio assume dizziness must be unrelated because the mouth and balance system seem far apart. In reality, they’re closer than commonly believed, especially when an upper back tooth is involved.
A person might notice that the room doesn’t spin exactly, but something feels off. Standing up may feel shaky. Walking may feel unsteady. Concentrating may become harder. When that happens alongside tooth pain, swelling, or signs of infection, a dental cause deserves serious attention.
Table of Contents
- Feeling Dizzy and Unwell? Your Toothache Could Be the Cause
- How a Dental Abscess Can Lead to Dizziness
- Warning Signs You Shouldn't Ignore
- Your Path to Relief at Amanda Family Dental
- A Holistic Approach to Your Recovery
- When and How to Get Help in Amanda and Surrounding Areas
Feeling Dizzy and Unwell? Your Toothache Could Be the Cause
A common story goes like this. Someone has a nagging upper toothache for days, maybe longer. Then the pressure spreads into the cheek or jaw, sleep gets worse, eating becomes difficult, and a strange dizzy feeling starts showing up.
That combination often creates confusion. Many people start by thinking of an ear problem, sinus issue, or blood pressure concern. Some schedule multiple medical visits before anyone looks closely at the tooth itself.
A documented clinical case showed exactly how easily that can happen. A young, otherwise healthy patient dealt with dizziness and unbalanced walking for four months before a dental exam revealed a chronic abscess near an upper second molar. After root canal therapy, the dizziness completely disappeared, according to this published case report on dizziness linked to an upper molar abscess.
Dental symptoms don’t always stay in the mouth. Infection, pressure, and inflammation can show up as head and balance symptoms first.
That’s one reason patients searching for can an abscessed tooth cause dizziness, emergency dentist, or dentist near me often need more than pain relief alone. They need a careful evaluation that connects the symptoms instead of treating each one as a separate mystery.
Why people often miss the connection
The confusion usually comes from how symptoms overlap. Dizziness can happen with sinus congestion, ear fullness, fatigue, dehydration, poor sleep, or stress. A dental abscess can contribute to several of those at once.
Common thoughts patients have include:
- “It’s probably just sinus pressure.” That may be partly true, especially with an upper tooth infection.
- “If it were my tooth, the pain would be unbearable.” Some abscesses cause intense pain. Others cause pressure, tenderness, or a dull ache.
- “Dizziness sounds too serious to come from a tooth.” In some cases, a tooth infection really is the missing piece.
For families in Amanda, OH and nearby Lancaster, Circleville, and Carroll, this matters because timely dental care can shorten the path to answers. A good exam doesn’t just look for cavities. It checks whether an infection, swelling, or hidden abscess could be affecting the rest of the head and body.
What this means for someone feeling off today
If dizziness appears with tooth pain, gum swelling, facial pressure, or a foul taste, it shouldn’t be brushed off. That doesn’t automatically mean the situation is dangerous, but it does mean the symptoms deserve prompt attention.
How a Dental Abscess Can Lead to Dizziness
A dental abscess is an infection, usually near the root of a tooth. Once infection builds pressure and inflammation in a confined area, nearby tissues can react. In the upper jaw, that reaction can affect spaces and structures involved in balance.
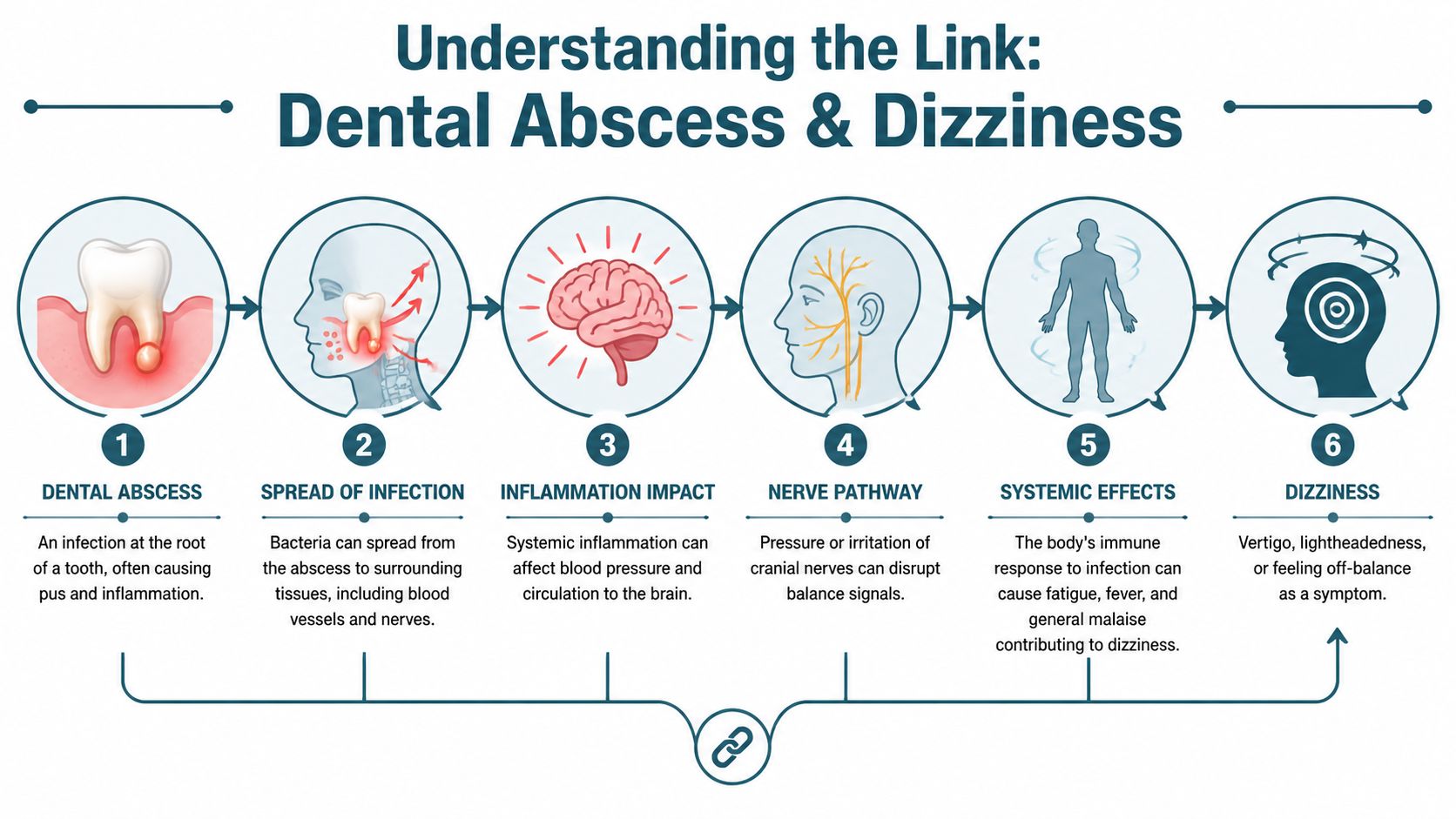
Why upper teeth matter so much
Upper molar abscesses are especially important because of where they sit. The upper molars attach directly to the maxillary sinus, and that sinus lies next to the inner ear and the vestibular system that controls balance. This clinical explanation of upper molar abscesses and dizziness describes how infection-related inflammation can create sinus pressure that directly disturbs the vestibular system.
A simple way to think about it is this. The infection may start in one small location, but the body responds across an entire neighborhood of connected spaces. When pressure and inflammation spread into the sinus area, balance can feel off even if the person wouldn’t describe it as classic spinning vertigo.
Three pathways tend to confuse readers most:
| Pathway | What happens | What it may feel like |
|---|---|---|
| Sinus involvement | Infection and inflammation increase pressure near the sinus | Facial pressure, ear fullness, imbalance |
| Circulation disruption | Inflammatory signals affect circulation and nearby tissues | Lightheadedness, “foggy” feeling |
| Inner ear irritation | Nearby balance structures get disturbed by pressure or spread | Unsteady walking, feeling off balance |
More than just pain
Pain itself can add another layer. A severe toothache can leave someone tense, nauseated, poorly rested, and not eating normally. Even without dramatic swelling, that combination can make the body feel shaky or faint.
In more serious situations, infection can also spread farther and contribute to systemic symptoms such as fever, fatigue, and generalized illness. Those symptoms can make dizziness worse.
Practical rule: If dizziness started around the same time as tooth pain, facial pressure, swelling, or a bad taste in the mouth, a dental cause belongs on the list.
Another detail matters here. Some abscesses don’t cause nonstop sharp pain. A person may mostly notice tenderness when biting, gum swelling, pressure under the cheekbone, or a sense that one side of the face feels “full.” That’s one reason people sometimes delay care. They don’t realize an infection can stay active even when the pain comes and goes.
For someone searching can an abscessed tooth cause dizziness while trying to decide whether to call a dentist in Amanda, OH, the answer is yes. The connection is anatomical, inflammatory, and in some cases very direct.
Warning Signs You Shouldn't Ignore
Some symptoms make the dental connection more likely. Others signal that the problem may be advancing and needs urgent attention.

Symptoms that often travel together
When dizziness comes from an abscessed tooth, people often notice a cluster of symptoms instead of only one. The pattern may include:
- Persistent tooth pain that throbs, aches, or worsens when chewing
- Sensitivity to hot, cold, or pressure
- Swelling in the gums, face, or jaw
- Bad taste or bad smell in the mouth, especially if infection is draining
- Facial pressure near the cheek or under the eye, often with upper back teeth
- Feeling run down with fatigue, low appetite, or nausea
- Unsteady balance or lightheadedness that seems worse when pain flares
A person may also feel ear pressure on the same side as the infected tooth. That can be especially misleading because it sounds like an ear problem first.
For readers who also deal with head pain, this related guide on tooth infection symptoms and headache patterns can help connect a few more dots.
One published case is especially helpful because it mirrors what many patients experience. The person went through multiple medical investigations for dizziness over several months, and the cause was only found during a dental exam. Once the chronic abscess was treated, the dizziness resolved. That kind of story is a reminder that unexplained balance symptoms sometimes need a dental workup, not just another round of non-dental testing.
Red Flags That Require Immediate Attention
Some symptoms go beyond “call soon” and move into “get help right away.”
Swelling that affects breathing or swallowing is not something to monitor at home.
Seek emergency care immediately if any of these are happening:
- Difficulty breathing or a tight feeling in the throat
- Difficulty swallowing or trouble handling saliva
- Rapidly increasing swelling in the face, jaw, or neck
- Severe illness with marked weakness, confusion, or worsening dizziness
- Fever with spreading swelling and obvious infection symptoms
This short video may help readers recognize when dental symptoms need prompt attention.
For less severe, but still concerning symptoms, an emergency dentist is usually the right first call. That includes situations where someone has tooth pain plus dizziness, swelling, facial pressure, or drainage from the gum.
Your Path to Relief at Amanda Family Dental
Once a dental abscess is identified, the goal is straightforward. Stop the infection, relieve pressure, and protect the patient’s overall health.
Research indicates that people with untreated dental infections have a 30% higher risk of dizziness, and clinical reports described in this review of dental infection and dizziness show that root canal therapy can be highly effective in resolving the symptom when infection is the cause.
What the visit usually involves
A focused dental visit for these symptoms often starts with a conversation about timing. When did the dizziness begin. Which tooth hurts. Is there swelling, drainage, or sinus pressure. Has eating, sleeping, or walking changed.
From there, the exam usually includes:
- A visual and clinical check of the painful area, surrounding gum tissue, and bite
- Digital X-rays to look for infection around the root or nearby bone
- A diagnosis discussion that explains whether the tooth can likely be saved or removed
- A treatment plan aimed at relieving the source, not only covering symptoms

Amanda Family Dental provides exams, digital X-rays, root canal therapy, tooth extraction, and other restorative care that may be part of treatment when infection is causing pain and dizziness.
Common treatment paths
If the tooth can be saved, root canal therapy is often the most direct way to remove infected tissue inside the tooth and keep the tooth in place. If the tooth is too damaged or the situation calls for removal, tooth extraction may be recommended instead.
A few patients also want to understand pain medication questions before treatment. For general educational background, FindMyScript's acetaminophen codeine guide explains important basics about that medication combination. Any medication decision still needs to follow a licensed clinician’s instructions.
The most important step is treating the source. Dizziness linked to a dental abscess usually doesn’t improve for long if the infection remains.
Patients who are anxious about treatment often feel better once they know what to expect beforehand. This page on how to prepare for a root canal appointment can make the process feel more manageable.
For people searching dentist in Amanda, OH, dentist in Lancaster, OH, dentist in Circleville, OH, or dentist in Carroll, OH, speed matters. An abscess usually doesn’t resolve on its own, and the longer it stays active, the more likely it is to keep disrupting daily life.
A Holistic Approach to Your Recovery
Treating the tooth is the central step, but full recovery often depends on more than the procedure itself. Dizziness can be intensified by sleep loss, dehydration, stress, and reduced food intake, especially when chewing hurts.
A more complete approach helps patients feel better sooner and more steadily. That matters because someone can still feel weak or off balance for a period even after the dental cause has been identified.
Why dizziness can linger even after the cause is found
Pain-related stress, poor sleep, and reduced eating can all worsen dizziness during a tooth abscess, according to this discussion of toothache-related dizziness and supportive care. In practical terms, the infection may be the spark, but the body’s response can keep the dizzy feeling going.
A person with a sore upper molar may avoid drinking because cold water hurts. That same person may sleep badly because pressure increases when lying down. By the next day, the body is dealing with infection, fatigue, and possible dehydration all at once.
Simple ways to support recovery
Helpful supportive care often includes:
- Hydration first by taking small, regular sips if normal drinking is uncomfortable
- Gentle nutrition with soft foods that are easier to tolerate when chewing hurts
- Better sleep setup by resting with the head slightly raised if pressure seems worse lying flat
- Calmer recovery habits such as limiting strenuous activity if dizziness is active
- Symptom tracking so changes in swelling, fever, or balance are noticed early
Recovery is usually smoother when patients treat the infection and the strain it has placed on the rest of the body.
This broader view of oral and overall health is why some patients find it useful to read more about the connection between oral health and whole-body wellness.
People often assume supportive advice is minor compared with the dental procedure. It isn’t. Small steps like hydration, nutrition, and rest can make a meaningful difference in how stable someone feels during healing. They also help the body tolerate treatment and bounce back more comfortably.
When and How to Get Help in Amanda and Surrounding Areas
The next step depends on the severity of symptoms. Some situations call for an urgent dental appointment. Others belong in the emergency room.
Call a dentist promptly if
A dental appointment should be arranged as soon as possible if dizziness appears along with signs of tooth infection such as pain, swelling, gum tenderness, drainage, or facial pressure.
A prompt call makes sense when someone has:
- Tooth pain plus dizziness that keeps returning
- Facial or gum swelling without breathing or swallowing trouble
- Pain when chewing or biting on one side
- A bad taste in the mouth that suggests drainage
- Pressure in the cheek or upper jaw near a back tooth
- An infected-looking tooth with worsening discomfort
For residents of Amanda, OH, Lancaster, OH, Circleville, OH, and Carroll, OH, this is the point to contact a local dental office rather than waiting to see whether it settles down.
Go to the emergency room if
Some symptoms should not wait for a routine dental opening.
Go to the ER immediately if there is:
| Emergency symptom | Why it matters |
|---|---|
| Trouble breathing | Swelling may be affecting the airway |
| Trouble swallowing | Infection or swelling may be spreading |
| Rapidly expanding swelling | The condition may be progressing quickly |
| Severe weakness or confusion | The body may be under significant stress from infection |
If the situation isn’t life-threatening but still feels urgent, calling an emergency dentist is the right move. A dental exam can determine whether the source is an abscess, whether root canal therapy or extraction is needed, and how to move toward relief safely.
People looking online for emergency dentist, dentist near me, or tooth extraction are often already at the point where waiting has become harder than getting checked. Dizziness alongside dental pain is one of those combinations that deserves action, not guesswork.
If dizziness is happening with tooth pain, swelling, or facial pressure, Amanda Family Dental is a local option for patients in Amanda, Lancaster, Circleville, and Carroll, Ohio who need prompt evaluation, digital X-rays, and a clear treatment plan. Reaching out for care can help identify the cause, relieve the infection, and get daily life feeling steady again.
