A bad tooth rarely waits for a convenient time. It starts as a nagging ache while eating dinner, a sharp jolt when drinking something cold, or swelling that makes it hard to ignore. By the time many people start searching for a dentist near me, they're not looking for a lecture. They want relief, answers, and a clear plan that doesn't make an already stressful situation feel worse.
For families in Amanda, OH, and nearby communities like Lancaster, Circleville, and Carroll, that stress often comes with a second worry. Will a tooth extraction hurt? Modern care is much different than people expect. Today's extractions are carefully planned, numbness is the standard, and the right approach depends on what the tooth and surrounding bone look like.
Patients also tend to judge a practice before they ever call, which is one reason local search listings matter. For anyone comparing offices online, these Google Business Profile optimization tips help explain why accurate hours, reviews, photos, and service details make it easier to find dependable local care fast.
Table of Contents
- Your Local Guide to Tooth Extraction in Amanda OH
- Understanding When a Tooth Needs to Be Removed
- The Tooth Extraction Process Simple vs Surgical
- Your Comfort-Focused Extraction Visit in Amanda
- Your Recovery A Week-by-Week Healing Guide
- Alternatives and Planning for the Future
- Understanding Extraction Costs and Payment Options
- Frequently Asked Questions About Tooth Extractions
Your Local Guide to Tooth Extraction in Amanda OH
A tooth extraction is one of the oldest procedures in dentistry. Evidence of active tooth removal has been found in prehistoric human skulls on every human-occupied continent, and writings associated with Hippocrates and Aristotle from roughly 500–300 BCE discussed removing teeth and wiring jaws, according to this history of oral surgery and extraction milestones. That long history matters for one reason. Tooth removal isn't a desperate improvisation. It's a well-established procedure that has become safer, more controlled, and far more comfortable over time.
That's important for anyone in Amanda, Lancaster, Circleville, or Carroll who feels uneasy hearing the words tooth extraction. Fear usually comes from not knowing whether the visit will be painful, rushed, or complicated. In reality, the process begins with diagnosis. The team looks at the tooth, the roots, the gumline, and what's happening around the area before recommending anything.
Practical rule: A tooth extraction should feel like a carefully planned health decision, not a surprise procedure pushed through in one appointment.
Some patients need urgent care because the tooth is actively painful. Others have a cracked tooth, a failed restoration, crowding, or advanced gum problems that make saving the tooth unrealistic. The right answer isn't always to remove it immediately, but when extraction is the healthiest option, clear planning lowers stress significantly.
What works for most anxious patients is straightforward communication and a step-by-step explanation of what's happening. What doesn't work is vague reassurance without specifics. People usually feel calmer when they know whether the tooth is likely a simple forceps extraction or a more involved surgical one, how numbness will be achieved, and what recovery will look like over the next several days.
For local patients searching for a dentist in Amanda, OH, or an emergency dentist near Lancaster, Circleville, or Carroll, the most useful next step is a focused exam. Once the source of pain is identified, treatment becomes much less intimidating.
Understanding When a Tooth Needs to Be Removed
Not every damaged tooth needs to come out. Dentists look first at whether the tooth can still be restored with a filling, crown, or root canal. Extraction enters the conversation when the tooth can't be predictably saved, when infection or damage has gone too far, or when keeping the tooth creates bigger problems for the rest of the mouth.

The most common reasons dentists recommend removal
A tooth may need to be removed for several different clinical reasons:
- Severe decay: Cavities can destroy too much healthy structure for a filling or crown to hold.
- Deep infection: An abscess or longstanding infection can threaten surrounding tissue and cause significant pain.
- Advanced periodontal disease: If the supporting bone and gum tissue break down too far, the tooth may become too loose to keep.
- Irreparable fracture: A break that extends below the gumline often leaves little dependable tooth structure to restore.
- Orthodontic planning: In select cases, removing a tooth creates the space needed to improve alignment and bite.
Across multiple studies, the leading reasons for extraction of permanent teeth were dental caries at 36.0% to 55.3% of cases and periodontal disease at 24.8% to 38.1%, according to this systematic review on reasons for permanent tooth extraction. That pattern shows something many patients don't realize. Extractions are usually a last resort, not a first choice.
When waiting usually makes things harder
A painful tooth sometimes settles down for a few days, which can give the impression that the problem is improving. Often it isn't. Pain can fade temporarily while infection, fracture, or bone loss continues underneath.
Here are signs that deserve prompt attention from an emergency dentist or general dentist:
| Concern | Why it matters |
|---|---|
| Swelling around a tooth | It may signal infection or pressure in the surrounding tissue |
| Pain with chewing | It can point to a crack, deep decay, or root problem |
| A tooth broken at the gumline | Restoring it may be difficult or impossible |
| A loose adult tooth | Supportive bone or gum tissue may be compromised |
A tooth doesn't need to be unbearable to justify treatment. If it's affecting eating, sleeping, or concentration, it's already interfering with daily life.
For patients in Amanda, OH and nearby towns, the key is getting the tooth evaluated before the situation turns into a larger emergency. Timely care can make treatment simpler, recovery easier, and the overall plan more predictable.
The Tooth Extraction Process Simple vs Surgical
The phrase tooth extraction covers two different procedures. One is a simple extraction, which is used when the tooth is visible and can be accessed above the gumline. The other is a surgical extraction, which is used when the tooth isn't easily accessible, is broken at the gumline, or needs to be removed in sections for safety.
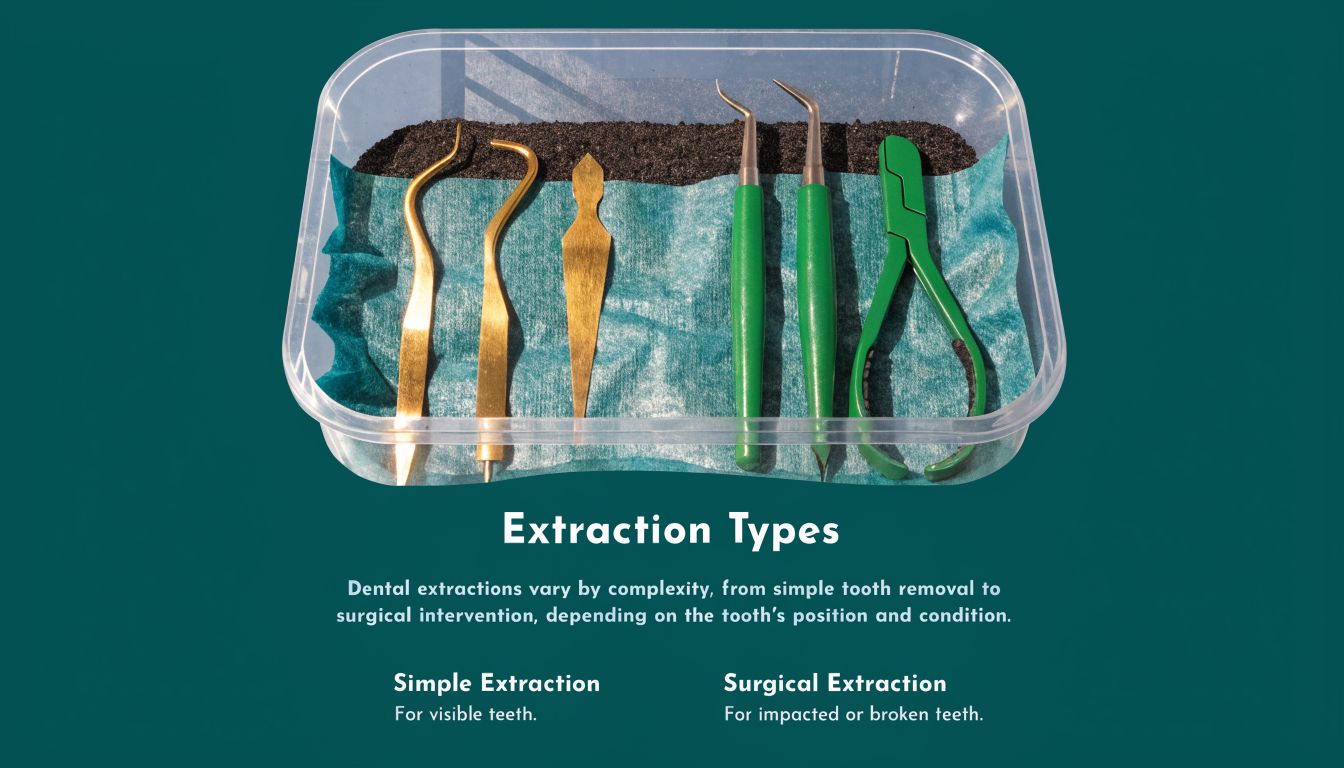
What makes an extraction simple
A simple extraction is generally appropriate when the tooth is fully visible and intact enough to grasp. The standard method uses an elevator to loosen the tooth and forceps to remove it. The clinician places the forceps as far down on the tooth as possible to improve control and reduce the chance of crown fracture. Rotational movement isn't used early on for teeth with non-round roots, because the roots and socket shape determine which directions are safest, based on this step-by-step explanation of simple and surgical extraction mechanics.
The goal isn't to yank a tooth out. The goal is to gently enlarge the socket, compress the surrounding cancellous bone, and sever the periodontal ligament so the tooth can be delivered with control.
When a surgical extraction is the safer option
A surgical extraction is chosen when a tooth hasn't fully erupted, has fractured at the gumline, or can't be removed predictably as one piece. In those cases, an incision is made to access the area, and the tooth may be sectioned so it can be removed safely.
That sounds more intimidating than it usually feels to a patient. The difference is mainly about access and control, not about punishment for having a “bad tooth.”
The method changes because the anatomy changes. A surgical approach often reduces risk when a simple pull would place too much stress on bone or soft tissue.
This short overview can help many patients visualize the difference before their appointment:
A simple way to compare the two approaches is below:
| Type of extraction | Usually used when | Main tools or access |
|---|---|---|
| Simple | Tooth is visible and intact | Elevator and forceps |
| Surgical | Tooth is inaccessible, broken, or impacted | Incision, direct access, possible sectioning |
Patients often assume that “surgical” means something has gone terribly wrong. Usually it means the dentist is choosing the more controlled route. For someone with a broken molar in Lancaster, an impacted wisdom tooth near Circleville, or a root fragment in Carroll, that distinction can make the experience safer and more comfortable.
Your Comfort-Focused Extraction Visit in Amanda
A lot of patients arrive for an extraction carrying the same worry. They are not just concerned about the tooth. They are concerned about how the appointment will feel minute by minute. At Amanda Family Dental, comfort starts before the tooth is removed. It starts with a plan, a clear explanation, and enough time to help people settle in.
The first part of the visit is careful evaluation. The goal is to understand what is happening below the gumline before treatment begins. Modern imaging helps identify root shape, nearby nerves, sinus position, and other details that can change how an extraction should be handled, as explained in this dental surgery reference on imaging and anatomic risk.
That step matters for patients with impacted teeth, curved roots, broken teeth, or upper back teeth that sit close to the sinus. It also helps answer a question I hear often. “Why does my neighbor's extraction sound simple when mine sounds more involved?” The answer is usually anatomy, not toughness or pain tolerance.
A comfort-focused appointment usually includes:
- A focused exam: We confirm which tooth is causing the problem and whether it can still be saved.
- Digital X-rays: These show root position, bone levels, and hidden factors that affect removal.
- A clear treatment plan: Patients learn what type of extraction is recommended, how the area will be numbed, and what support they will need afterward.
- Realistic timing: The American Dental Association notes in this patient guide to tooth extractions that timing depends on the tooth and the difficulty of the case, so straightforward visits are often fairly quick while surgical cases can take longer.
Comfort during the procedure depends on good anesthesia and good communication. Local anesthesia numbs the area so patients should not feel sharp pain. Pressure is still possible, especially with back teeth, but pressure is a different sensation. When patients know that ahead of time, they usually feel far less alarmed.
Some patients need more than numbness alone to feel comfortable. Anxiety, a strong gag reflex, past difficult dental visits, or the stress of an urgent appointment can all make treatment harder than it needs to be. Patients who want to review added comfort options can learn more about our sleep dentistry services during treatment planning.
In a small community practice, that conversation matters. People from Amanda, Lancaster, Circleville, and nearby towns are often seeing familiar faces when they come in. That local connection does not replace clinical skill, but it does change the experience. Patients tend to relax more when they know the team will slow down, answer the uncomfortable questions plainly, and stop if they need a moment.
Clear explanations are one of the best comfort tools we have. If a patient knows when they will feel numb, when they may notice pressure, and how we will respond if anything feels too intense, the procedure becomes much more manageable. That is the standard we aim for at Amanda Family Dental. Care that is clinically sound, calm, and considerate from the first conversation through the last instruction before heading home.
Your Recovery A Week-by-Week Healing Guide
The ride home is often when the questions start. Is this amount of bleeding normal? When will eating feel easier? What if the pain gets worse instead of better? A clear recovery plan settles a lot of that worry.
Healing starts with a blood clot forming in the empty socket. That clot covers the bone and nerve endings while your body begins repairing the area. If the clot breaks down or comes out too soon, patients can develop dry socket, a painful complication described by the American Dental Association's guidance on dry socket.
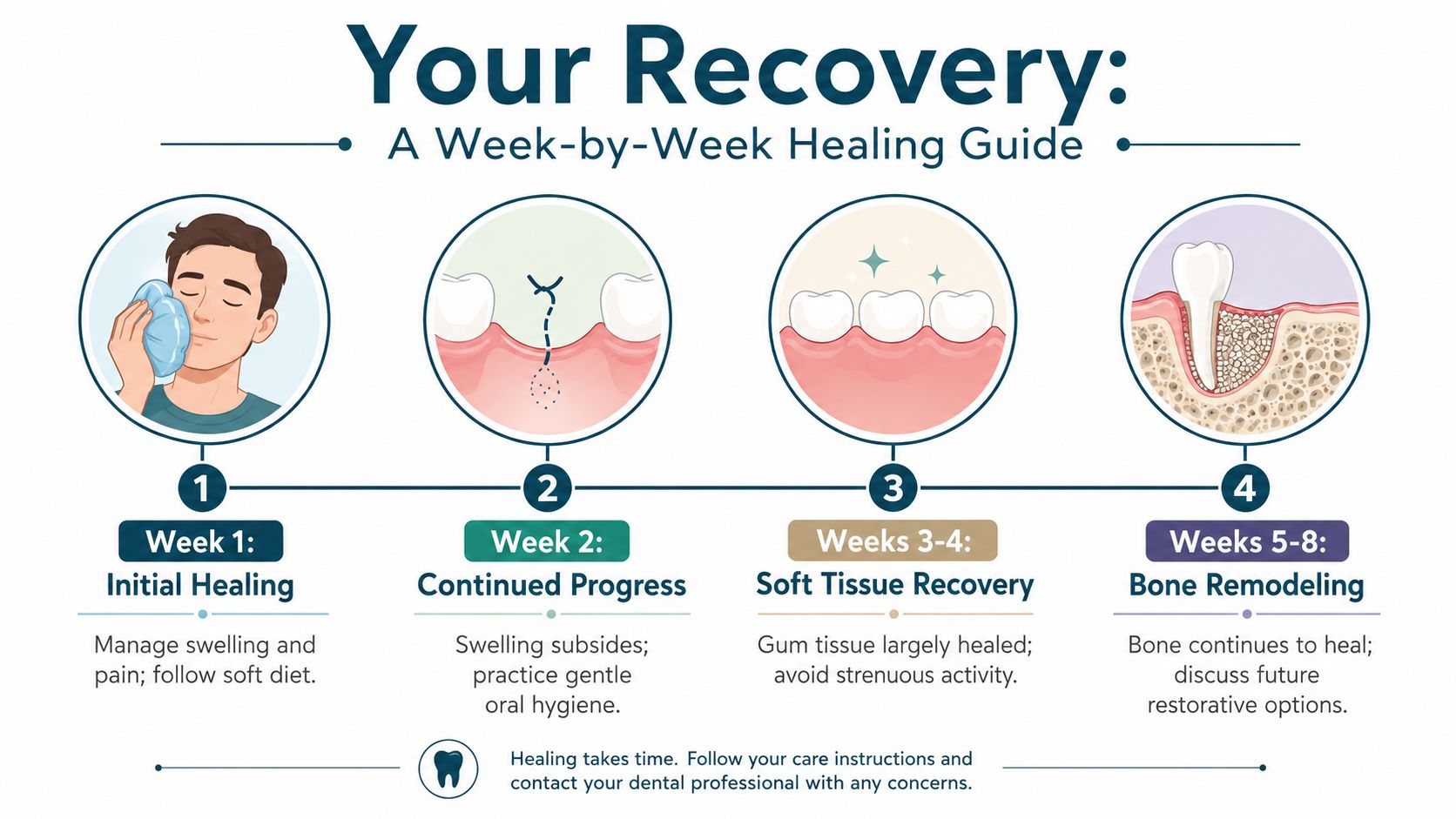
The first twenty four hours
Day one is about protecting the site. Oozing, tenderness, and mild swelling are common. Patients usually do best when they rest, keep pressure on the gauze as directed, and avoid anything forceful in the mouth.
A few basics make a real difference:
- Protect the clot: Avoid spitting hard, drinking through a straw, smoking, or vigorous rinsing.
- Keep food simple: Choose soft, cooler foods that are easy to chew away from the area.
- Stay ahead of discomfort: Use prescribed or recommended pain relief exactly as directed.
- Clean carefully: Brush and floss the other teeth, but do not scrub the extraction site.
The goal is simple. Keep the area quiet so the body can get started.
Days two through seven
This is the stretch where patients usually begin to feel more like themselves. Swelling often peaks early, then starts to come down. Soreness should gradually ease, even if the area still feels tender during eating or brushing nearby.
Dry socket tends to show up during this window, which is why changes in pain matter more than pain alone. A dull ache that improves is expected. Pain that becomes sharper, more throbbing, or harder to control after a few days deserves a call to the office.
| What's usually normal | What deserves a call |
|---|---|
| Mild soreness that slowly improves | Pain that worsens after initial improvement |
| Light swelling that starts settling down | Throbbing pain several days after the extraction |
| Tender chewing near the area | Bad taste, unpleasant odor, or concern the clot was lost |
| Slow return to regular meals | Pain medicine not giving enough relief |
At Amanda Family Dental, we would rather hear from a patient early than have them sit at home wondering if they should wait another day.
Week two and beyond
By the second week, the gum tissue is usually closing over and daily routines feel much easier. Surgical extractions, infected teeth, and wisdom tooth removals can take longer to settle than a simple extraction. That difference is normal, but healing should still move in the right direction.
Some patients also want to know what happens after the site closes. If the extracted tooth will need to be replaced, our tooth replacement options after extraction page explains the next steps in plain language.
Good recovery is rarely dramatic. It is steady. The area gets less sore, eating gets easier, and each day asks a little less of you. That is the pattern we want for our Amanda neighbors, along with clear instructions and a local office that is easy to reach if anything feels off.
Alternatives and Planning for the Future
A tooth extraction should never feel disconnected from the bigger picture. The immediate problem may be pain, infection, or a broken tooth, but the long-term goal is a healthy bite, comfortable chewing, and a plan for the space that's left behind.
Extraction is not always the first answer
Dentists typically consider whether a tooth can be saved before recommending removal. In some cases, a root canal, crown, or other restorative treatment may still be the better choice. That's especially true when the tooth has enough healthy structure left and the surrounding bone support is still solid.
When extraction is the right call, technique matters. Modern atraumatic methods are designed to preserve as much surrounding jawbone as possible, which is especially useful when future implant placement is under consideration, according to this overview of atraumatic extraction and implant planning.
Replacing a missing tooth matters
Once a tooth is removed, the next question is whether to replace it. The answer depends on the location of the tooth, the bite, cosmetic concerns, and the patient's goals. In many cases, replacement helps restore chewing function and supports long-term oral stability.
Common options include:
- Dental implants: Often considered when patients want a fixed replacement and bone preservation matters.
- Bridges: A practical option in some cases when neighboring teeth and bite conditions make sense for support.
- Partial dentures: Sometimes useful when several teeth are missing or when a removable option fits the treatment plan better.
Patients who are comparing next steps after a tooth extraction can review tooth extraction and replacement options to understand how removal and restoration fit together.
A useful mindset shift is this: extraction is not the end of treatment. It's often the point where treatment turns from pain control to rebuilding. For adults searching dental implants near me in Amanda, Lancaster, Circleville, or Carroll, the quality of the extraction itself can influence future choices. Bone preservation today can make tomorrow's restoration simpler and more predictable.
Understanding Extraction Costs and Payment Options
Cost matters, especially when a tooth starts hurting unexpectedly. Most patients aren't just asking what a tooth extraction costs. They're asking what affects the fee, whether insurance may help, and how to move forward without delaying care for financial reasons.
What changes the cost of care
There isn't one flat price that fits every extraction. Fees can vary based on the complexity of the case and what the visit requires. A visible tooth removed with a simple forceps approach is different from a broken or impacted tooth that needs a surgical technique.
Common cost factors include:
- Procedure type: Simple and surgical extractions involve different levels of time, access, and technique.
- Imaging needs: Digital X-rays are often necessary to plan care safely.
- Sedation or comfort services: Some patients need more than local anesthesia.
- Follow-up treatment: Bone preservation or future replacement planning can affect the larger treatment budget.
For patients trying to understand how insurance claims and dental billing usually work behind the scenes, this overview of Happy Billing dental support gives a helpful look at the administrative side of dental care.
How families often make treatment work
The most helpful approach is transparent conversation before treatment begins. Patients should know what the office recommends, what parts may involve insurance, and what alternatives exist if care needs to be phased.
Amanda Family Dental offers payment information and financing details through its financing page, which is useful for patients comparing timing and affordability. The practice also offers a Power Plan Membership, which may help some families manage ongoing dental care when traditional insurance isn't the only path they want to rely on.
Good treatment planning includes financial planning. Patients make better decisions when they understand both the clinical need and the payment path.
For households in Amanda, OH and nearby Lancaster, Circleville, and Carroll, the goal is straightforward. Get the pain handled, understand the options, and avoid putting off necessary care because the cost conversation never happened clearly.
Frequently Asked Questions About Tooth Extractions
Patients usually have a few final questions even after the diagnosis is clear. That's normal. A tooth extraction can still feel intimidating when someone is trying to line up work, childcare, meals, and recovery all at once.
Will the extraction itself hurt
The extraction itself shouldn't feel sharp if the area is properly numbed. Most patients notice pressure, movement, and odd sensations more than pain. That's one reason a careful explanation before treatment helps so much. Knowing what pressure feels like keeps it from being mistaken for something dangerous.
If a patient is highly anxious, it's worth discussing comfort options before the appointment begins. Anxiety often makes every sensation feel bigger than it is.
How much time should patients plan to take off
That depends on the tooth, the difficulty of the procedure, and the kind of work the patient does. Desk work may be easier to return to sooner than physically demanding work. Some people feel ready the next day after a simple extraction, while surgical cases may need a bit more downtime.
The smartest approach is to avoid overcommitting the day of treatment. Keeping the schedule light reduces stress and gives the body room to recover.
Is it okay to leave the space empty
Sometimes a missing tooth creates little immediate disruption. Other times it affects chewing, appearance, or the way nearby teeth function. Back teeth and front teeth raise different concerns, and not every space needs the same solution.
A gap should be evaluated as part of a long-term plan, not ignored by default. Replacement may support function, appearance, or future stability depending on the case.
What symptoms mean the office should be called
Patients should reach out if something feels off, especially if recovery seems to reverse direction. A short list makes that easier to judge:
- Pain is increasing instead of improving: That pattern deserves attention.
- Swelling seems to worsen rather than settle: It may need to be evaluated.
- The area feels difficult to manage with the given instructions: Patients shouldn't wait and hope.
- Something doesn't seem normal: A quick call is better than guessing.
One final reassurance matters. A tooth extraction is common, but it should still feel personal. The best dental care balances skill with calm communication, especially for patients who are nervous, embarrassed, or arriving in pain for the first time.
If tooth pain, swelling, or a broken tooth is making daily life harder, Amanda Family Dental provides local care for patients in Amanda, Lancaster, Circleville, and Carroll, Ohio. Scheduling an exam is the fastest way to learn whether the tooth can be saved, whether extraction is the right step, and what treatment and replacement options fit the situation.
